Those with esophageal inflammation experiencing difficulty swallowing or frequently getting food stuck in their esophagus may be diagnosed with eosinophilic esophagitis. This relatively newly recognized disease can result in damage to the lining of your esophagus, which can worsen over time if untreated.
Here’s everything you need to know about eosinophilic esophagitis.
What Is Eosinophilic Esophagitis?
Eosinophilic esophagitis (EoE) is a chronic immune system disease that develops when a type of white blood cell called an eosinophil collects in the lining of the esophagus sometimes as a reaction to certain foods, allergens, or acid reflux.
The condition can inflame or damage the esophageal tissue, which can lead to dysphagia (difficulty swallowing) or impaction (food gets stuck in your esophagus during swallowing).
Eosinophilic esophagitis was first identified in 1978 and classified as a distinct clinical entity in 1993. Since its discovery, it is now considered a major cause of dysphagia and food impaction.. Research is still ongoing, but there has been a notable increase in the number of people diagnosed with EoE throughout the last 10 years, suggesting the condition is becoming more common or identifiable.
Causes
Eosinophilic esophagitis is caused by an allergic response to a food or outside substance in which the white blood cell eosinophils—normally found in the digestive tract—accumulate in the esophagus and release substances into surrounding tissues, causing inflammation.
There are a wide variety of risk factors associated with developing EoE, including:
- Age
- Allergies
- Asthma
- Climate
- Genetics & Family History
- Sex
EoE is most common in males, and can affect both children and adults. Its current prevalence in North America is one in every 1,000 adult individuals.
Most of those diagnosed with EoE have a history of allergic disorders, including asthma, allergic rhinitis, allergic conjunctivitis, or food allergies. The foods most commonly associated with EoE reactions include milk, eggs, wheat, soy, peanuts, beans, rye, and beef.
Symptoms
Typically, EoE symptoms develop when the lining of the esophagus reacts adversely to allergens, such as food or pollen. Eosinophils multiply in the esophagus and produce a protein causing inflammation, which can lead to scarring and narrowing of the lining of the esophagus.
EoE manifests differently, depending on age. In children and teenagers, symptoms can range from:
- Difficulty Eating
- Vomiting
- Abdominal pain
- Dysphagia
- Food Impaction
- Poor Growth & Malnutrition
In adults, EoE is more frequently identified in males than females, with the average ages of those diagnosed between 30 and 50 years. Adults can experience:
- Dysphagia
- Food Impaction
- Chest Pain
- Regurgitation
Diagnosing Eosinophilic Esophagitis
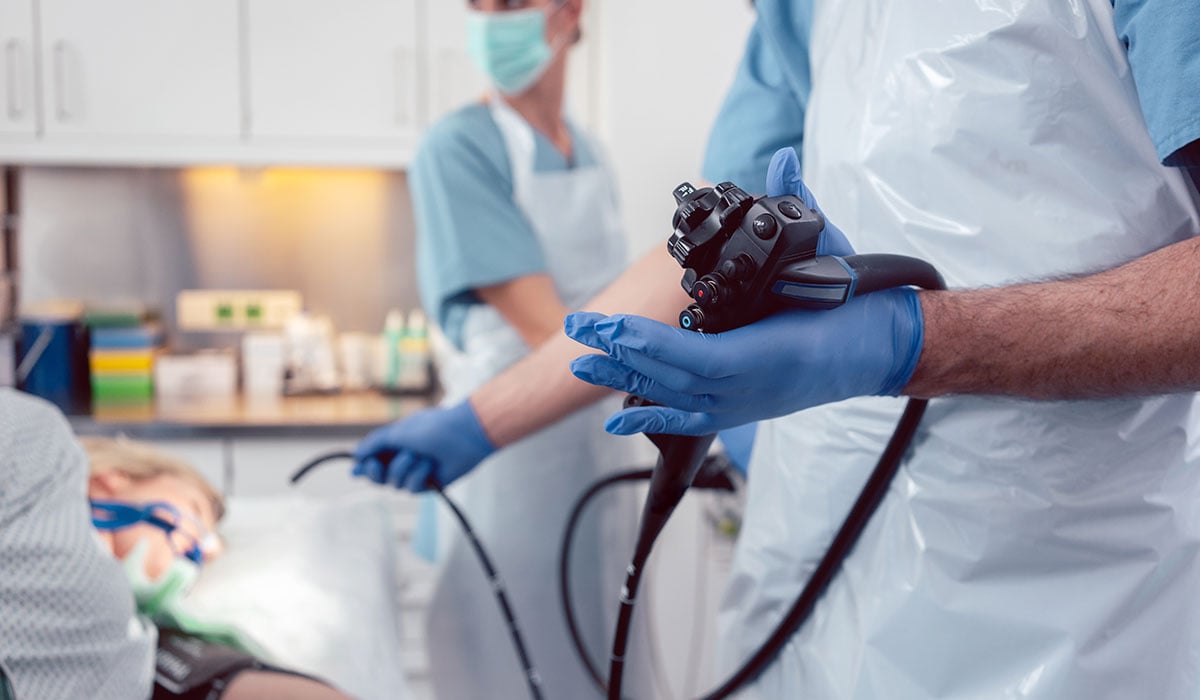
There are several ways a doctor can diagnose EoE, but the first step is conducting an upper endoscopy with biopsies of the esophagus to identify the presence of eosinophils, or see if the esophagus is scarred or inflamed.
Treatment Options
While there is currently no cure for EoE, your doctor can recommend treatments to help manage symptoms and avoid further damage. The two main methods are medicinal and dietary.
The U.S. Food and Drug Administration (FDA) has yet to approve medications for the treatment of EoE, however, several have proven effective at addressing symptoms and reducing the number of eosinophils in the esophagus. These include:
Proton pump inhibitors (PPIs) that block and reduce stomach acid production, which can give any damaged esophageal tissue time to heal. Corticosteroids are helpful in controlling inflammation by treating the inner lining of the esophagus on contact.
There are also a number of dietary options which can be effective at addressing symptoms. These include eliminating specific foods and allergens from your diet. Such regimens have proven to be very helpful in treating EoE, but can often be difficult to follow. Research is underway to discover additional alternatives for new effective treatment.