When you suffer from gastroesophageal reflux disease (GERD), also known as chronic heartburn or acid reflux, finding the right treatment can be tricky. While there’s no shortage of internet advice on at-home treatments and alternative therapies, the truth is that GERD is best treated with the help of a professional.
Here’s what you need to know about GERD treatment.
What is GERD?
GERD is a digestive disorder that affects the lower esophageal sphincter (LES), the ring of muscles that separates the esophagus from the stomach. When the LES operates normally, it opens to allow food to pass through to the stomach and closes to prevent stomach acid from entering the esophagus.
With GERD, stomach acid flows back into the esophagus, irritating the esophageal lining and causing heartburn or acid reflux. According to the Mayo Clinic, the threshold for a GERD diagnosis is when you have “mild acid reflux that occurs at least twice a week, or moderate to severe acid reflux that occurs at least once a week.”
What causes GERD?
GERD can be caused by any number of factors, including:
- A hiatal hernia, wherein the stomach protrudes through the diaphragm (the muscle separating the heart and lungs from the abdomen), increasing the likelihood that stomach acid will pass through to the esophagus
- Pregnancy, thanks to hormones that slow down digestion and the growth of the uterus, which can push the stomach up into the diaphragm
- Trigger foods such as garlic, onion, spicy foods, chocolate, fried foods, and alcohol, which make the LES “lazy”
- Weight gain and/or obesity, which can push the stomach up into the diaphragm and esophagus
How do you get diagnosed?
To get an official diagnosis, your doctor will review both your symptoms and your medical history. If that’s not enough to determine whether or not you have GERD, they then may perform one of the following procedures:
- X-rays, though only one-third of patients with GERD “have radiological signs of esophagitis” (more commonly known as esophageal inflammation) which includes ulcers, striations, and hiatal hernias, according to an article published by American Family Physician
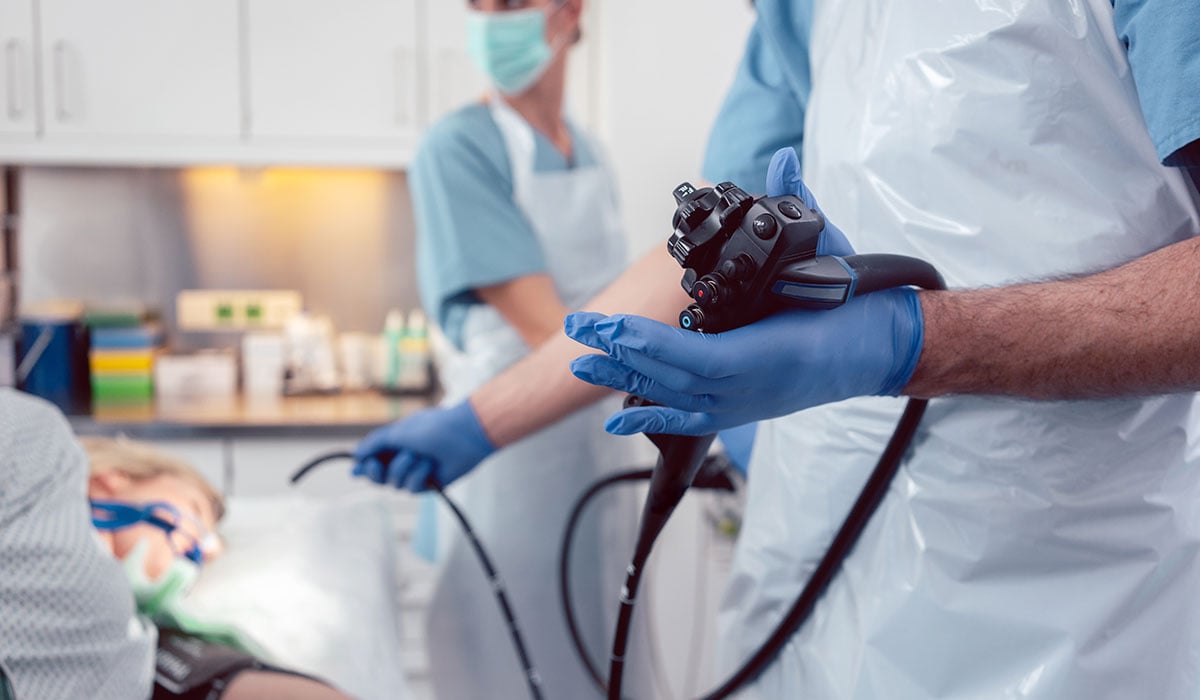
- An upper endoscopy, wherein a qualified professional will insert a small tube into your esophagus to examine the LES and stomach for signs of GERD
How do you treat GERD?
Left untreated, GERD can lead to Barrett’s esophagus, which in turn, increases the risk for esophageal cancer, so it’s important to treat your symptoms quickly.
Treatment is a stepped process, and depending on the severity of your symptoms, you either step-up treatment from least to most restrictive measures, or you step down from most to least restrictive.
For example, your doctor might ask you to make slight adjustments to your eating schedule, or ask you to go on an elimination diet to determine what, if any, trigger foods exacerbate your gastric distress. Finally, some doctors will recommend surgical options in extreme cases.
Treatment plans are highly individualized and should always be developed in conjunction with your doctor rather than solely based on internet research. After all, there’s no shortage of articles out there recommending homeopathic remedies without scientific evidence to back up their claims.
Here are the ways you can treat the digestive disease.
Make key lifestyle changes.
There is ample evidence to show the following habit changes can help treat symptoms:
- Wait to exercise at least two to three hours after eating. (Going for a walk after dinner is all right, but vigorous exercise should be delayed to prevent acid backflow.)
- Elevate the head of your bed six to nine inches and sleep on an incline. (Using pillows is not enough to create the uniform support needed to alleviate symptoms, so either use a foam wedge under your mattress or raise your bed frame’s feet near the head of your bed.)
- Do not lie down for at least three hours after a meal.
- Quit smoking tobacco products, which can both cause and exacerbate acid reflux.
- Ask your physician about dietary modifications.
If these simple lifestyle changes don’t work or aren’t doing enough, studies show weight loss can help to alleviate pressure on your organs. Weight management is often thought of as the first line of defense for GERD, as being overweight is one of the most common causes of the disease.
Eliminate trigger foods.
Part and parcel of treating GERD is determining whether or not you have trigger foods. According to the American Society for Gastrointestinal Endoscopy, trigger foods can make your LES lazy (affect its ability to close properly).
The following foods are common triggers:
- Caffeine, which relaxes the LES, preventing it from fully closing
- Chocolate, which contains a chemical called methylxanthine, similar to caffeine
- Spicy foods
- Acidic foods such as tomatoes and citrus fruits
- Fried foods, which slow digestion and relax the LES
- Mint
For more extreme cases of GERD, your doctor may suggest eliminating most or all trigger foods—independent of whether or not your doctor recommends weight loss—then slowly adding them back into your diet to both determine what exacerbates your symptoms and give your esophagus time to recover.
Use over-the-counter medication.
There are several OTC treatment options. Depending on your needs and the severity of your symptoms, your doctor may recommend the following:
- Antacids, which counteract stomach acid by coating the stomach with alkaline chemicals. These are usually a first-defense medicine, as they start working immediately. They help with immediate symptom relief but do nothing to prevent future symptoms.
- H2 blockers, which reduce acid production. H2s don’t act as quickly as antacids, but can offer more long-term relief and help aid the healing process for an inflamed esophagus.
- Proton-pump inhibitors, which block the site of stomach acid production and take several days to start working.
If OTC meds don’t work, use prescription meds.
There are prescription-strength H2 blockers and proton-pump inhibitors on the market, which your doctor may prescribe based on your needs.
Depending on the severity, your doctor might suggest surgical options.
Finally, if lifestyle and medical interventions are not helping, your doctor might suggest a surgical procedure.
- Fundoplication is a surgical procedure that wraps “the top part of the stomach around the end of the esophagus to reinforce the [LES].” According to the Society of American Gastrointestinal and Endoscopic Surgeons, this can be performed by making a long incision along the upper abdomen or using laparoscopic techniques to minimize the invasiveness and recovery time of the procedure.
Gastroenterology Associates can help restore you and your family to optimal digestive health, and is conveniently located adjacent to Long Island Center for Digestive Health (LICDH), a non-hospital outpatient facility committed to providing high-quality endoscopic and colonoscopic services. For more information or to schedule an appointment, contact us today!
Topics: gastroenterology associates