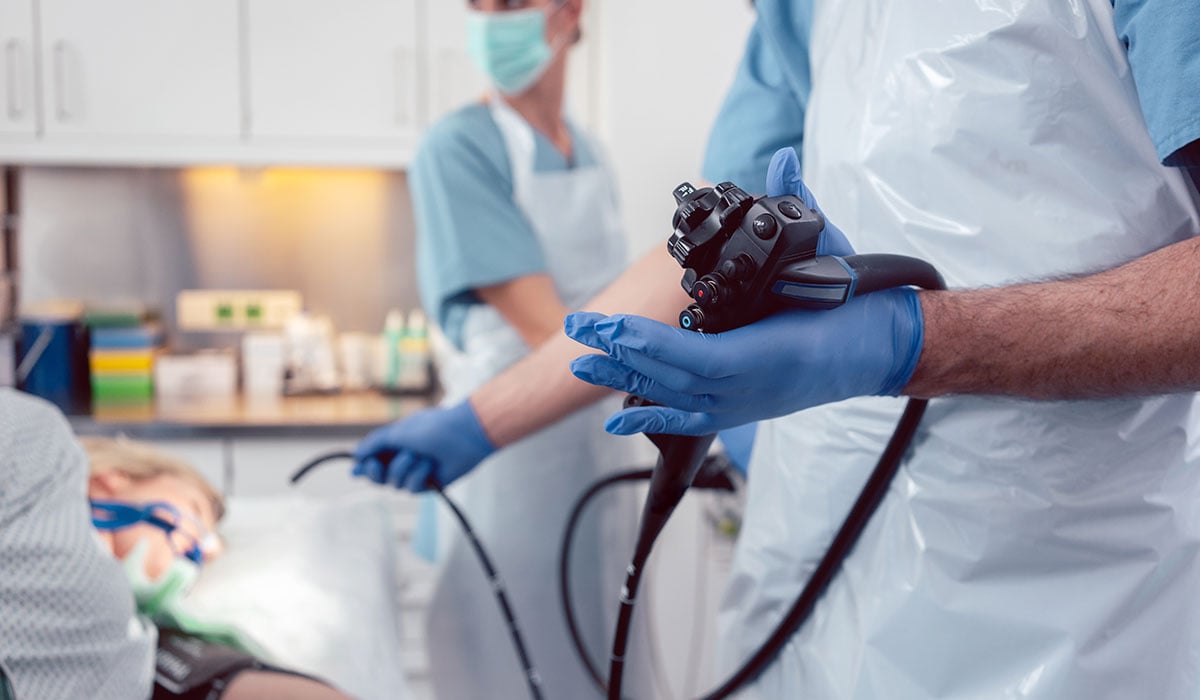
An upper endoscopy (or EGD) is a simple and safe procedure that benefits the lives of millions of Americans each year. Still, we know that scheduling an upper endoscopy could be intimidating, so we put together some information to shed light on the procedure and preparation guidelines to alleviate some of your worries.
What is an Upper Endoscopy?
An upper endoscopy, also known as an EGD (esophagogastroduodenoscopy), is a surgical procedure performed by gastroenterologists that helps to diagnose and treat certain gastrointestinal diseases and disorders. The scope of bodily coverage provided by this procedure includes your esophagus, stomach, and the first part of your small intestine, called the duodenum.
The procedure calls for a thin, flexible tube (called a gastroscope) to be lowered via the mouth, down through the esophagus, into the stomach, and to the duodenum. The gastroscope comes equipped with a small light and video camera on one end, which projects the images seen by the tube onto a monitor outside of your body.
Depending on your reasons for needing an endoscopy, a gastroscope may have tools attached in order to:
- Sample tissue for a biopsy
- Remove food that may be stuck in your GI tract
- Perform added procedures, such as endoscopic surgery, laser therapy, or opening a narrowed area
Why Get an Upper Endoscopy?
If you find yourself inexplicably suffering from any of the following symptoms:
- Trouble swallowing (dysphagia)
- Heartburn
- Sudden weight loss
- Upper belly pain or chest pain
- Continuous vomiting
The procedure could determine whether you have a GI disorder, like GERD (gastroesophageal reflux disease), Celiac disease, esophageal or intestinal strictures, or Crohn’s disease, all of which could be identified and treated by getting an EGD.
Why Not Get an X-Ray?
An EGD provides more accurate readings than an X-ray, especially for identifying problems like inflammation, ulcers, or tumors. The scope of an EGDs utility is much greater than that of an X-ray. Accessories may be attached to the gastroscope that allow your doctor to not only diagnose, but possibly simultaneously treat your condition.
For instance, your doctor may stretch narrowed areas, whether from strictures or Schatzki ring, or stop upper GI bleeding caused by ulcers tearing the lining of your stomach or esophagus. EGDs also allow for tissue biopsies and polyp removal, which are not possible during an X-ray.
What You Need to Know: Dietary Requirements and After-Care
To prepare for an EGD, you’ll be instructed to refrain from certain food and drink for a short time leading up to your procedure.
Approved liquids:
- Gatorade
- Pedialyte or Powerade
- Coffee or tea (no milk or non-dairy creamer)
- Carbonated and non-carbonated soft drinks
- Clear fruit juice (apple juice, white cranberry, or white grape juice)
- Jell-O, popsicles (NO red or purple)
Restricted liquids:
- Chicken, beef, or vegetable broth
- Red or purple items of any kind
- Alcohol
- Milk or non-dairy creamers
- Juice with pulp
- Hard candy
- Any liquid you can’t see through
If you are diabetic, please speak with your doctor about proper nutrition and about insulin administration before the day of your EGD. To prevent letting your blood-sugar drop too dramatically, you may be instructed not to take your oral medication or insulin until after a post-procedure meal.
Post-EGD Care
You’ll need a driver 18 years or older to accompany you to your appointment and immediately after your EGD, but it is also requested that they remain present for entirety of the three-to-four hour procedure. Since the anesthetic may leave you with temporarily impaired judgement, you can’t be released on your own to walk, or even to use public transportation like a bus or cab.
To prevent choking, you’ll be withheld from food and drink until your gag reflex returns. It is normal to feel gassy and/or to have a sore throat/pain swallowing in the days immediately following the procedure.
However, you should contact your doctor if you experience any of these symptoms in the days after your EGD:
- Fever or chills
- Redness, swelling, or bleeding or other drainage from the IV site
- Belly pain, nausea, or vomiting
- Black, tarry, or bloody stools
- Trouble swallowing
- Throat or chest pain that gets worse