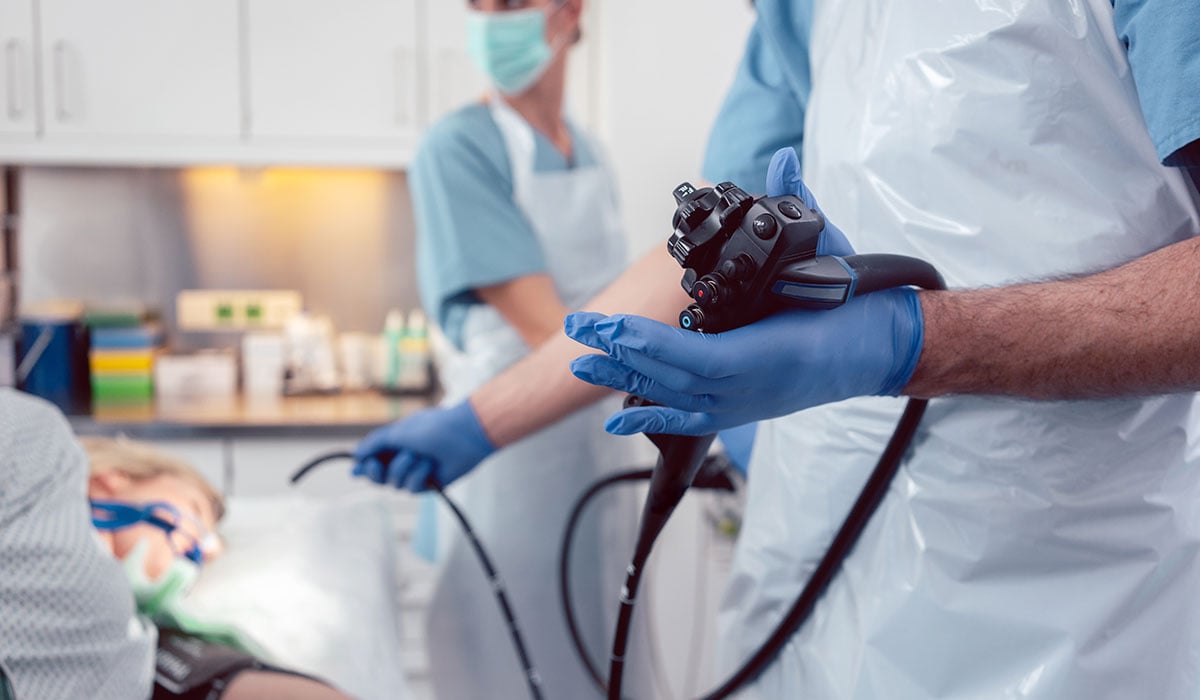
If you’re looking to address a specific medical concern or reach a higher-risk age group, your doctor may suggest a colonoscopy. While it may seem daunting at first, this procedure is quick, safe, and highly effective at identifying and locating issues within the colon and rectum.
Whether preparing for an upcoming colonoscopy, or just curious about what it entails, here’s what you need to know.
What Is a Colonoscopy?
Colonoscopies are procedures commonly performed when screening for colorectal cancers and colon polyps, as well as other issues with the large intestines.
It involves a gastroenterologist or colorectal surgeon inserting a colonoscope—a long, flexible tube with a small video camera on the end—into a patient’s rectum to inspect their entire colon for abnormalities.
When Are They Used?
Colonoscopies are frequently utilized to check for colorectal cancers, however a doctor may recommend the technique if there are any signs of rectal bleeding, chronic constipation, or diarrhea and other intestinal problems.
The American Cancer Society also advises adults between the ages of 45 and 75 to undergo regular colonoscopy screenings every 10 years or so—as this is the range when people are at the highest risk of developing colon cancer.
How to Prepare for Your Procedure
To prepare for your colonoscopy, there’s a list of actions your doctor will instruct you to follow.
If you take medication or iron supplements for certain issues including diabetes, high blood pressure, or heart conditions, your doctor may require you to adjust your dosages or cease them temporarily. You’ll also be asked to avoid certain anticoagulants, or other medications that thin the blood.
Prior to your colonoscopy, your doctor may ask you to adhere to a specific dietary regimen, avoid solid foods, and only drink clear liquids, the day before your exam. You may be required to refrain from eating or drinking that day.
Your doctor may request you use a laxative or enema kit the night before or morning of your procedure to empty your colon and ensure there’s as little residue as possible that may obscure results.
What Should You Expect From Your Procedure?
During the colonoscopy, patients will be asked to change into a medical gown and are given a sedative to minimize any discomfort.
The doctor will insert a colonoscope into the rectum, reaching the entire length of the colon. The camera transmits images to an external monitor, enabling the doctor to conduct a clear and thorough inspection.
The device contains a channel tube, which enables the doctor to inflate the colon with gas for a better view of its inner lining. If needed, the doctor can also take a tissue sample, or directly remove polyps or abnormal tissue.
The entire procedure should typically last between 20 to 30 minutes.
Patients should arrange to get a ride home afterward, and are advised to not drive or return to work to give the sedative time to completely leave their systems.
Depending on the results of the colonoscopy, patients may be advised to temporarily follow a certain diet, particularly if the doctor removed tissue or polyps.
Results & Next Steps
If normal and the doctor doesn’t find any issues or abnormalities, they’ll inform you and recommend another colonoscopy in 10 years if you’re at average risk for colon cancer, or more frequently if you have a history of polyps or other issues.
If the doctor does find issues such as polyps or abnormal tissue, they can be removed during the colonoscopy and sent to a laboratory to determine whether they’re cancerous. They may recommend a followup colonoscopy if they identify multiple polyps, those larger than a centimeter, or polyps and tissue with potentially cancerous characteristics.
What Are Potential Risks & After Effects?
Patients can often experience cramps, bloating, or gassiness in the hours following the exam, and they may see a small amount of blood in their first bowel movement. This generally isn’t cause for concern, but persistent bleeding, blood clots, abdominal pain, and fever are signs to consult your doctor.
Colonoscopies are typically very safe, but there are a few potential risks or complications, including adverse reaction to the sedative, perforation of the colon or rectal wall, or bleeding.
Gastroenterology Associates specializes in providing high-quality digestive healthcare. We are conveniently located adjacent to Long Island Center for Digestive Health (LICDH), a New York State-licensed, non-hospital outpatient facility dedicated to providing high-quality endoscopic and colonoscopic services. For more information or to schedule an appointment, contact us today!